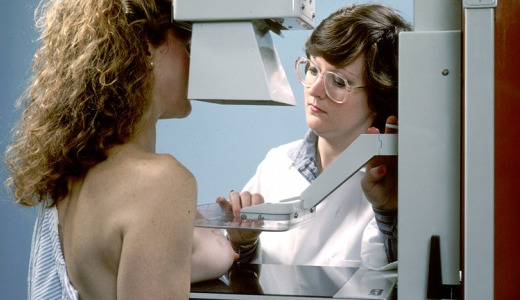
For the past 25 years many women have been wedded to the idea of having a mammogram and a manual breast examination by their doctor every year starting at age 40, and doing monthly self-examinations. Now new guidelines have turned life upside down.
On Nov. 16 the United States Preventive Services Task Force announced new guidelines for breast cancer screening and detection which include the recommendation that women receive their first mammogram at age 50, followed by mammograms every other year until age 75. Further, recommendations for monthly self-breast examinations were discontinued. These guidelines were informed by research that indicate younger women were being over-tested and over-treated as a result of false positive findings. Previously, women were advised, starting at age 40, to have yearly mammograms and yearly breast exams by a physician and to do self-breast examinations monthly.
The task force researchers believe that mammography in women younger than age 50 is often inaccurate, and falsely identifies normal tissue as possible tumors. Also, mammograms can find slow-growing cancers that will never cause a problem. These findings result in further testing, biopsies and even surgery, chemotherapy and/or radiation therapy, all of which may be unnecessary.
Present technology is not really suited to younger women’s breasts. The tissue in younger breasts tends to be denser than that of post-menopausal women. This density makes identification of cancerous lesions by current mammography techniques difficult. Thus, a biopsy, which scars the breast, may be performed. The residual scar tissue from a biopsy can make future mammography even more difficult. Women may unnecessarily receive chemotherapy and/or radiation treatment, the side effects of which can be terribly damaging, possibly leaving a woman sterile and at increased risk for other cancers.
On the flip side, even though it is less common in younger women, breast cancer tends to be more aggressive with a lower survival rate: 81 percent for women younger than 45, compared with 86 percent for women older than 65.
After lung cancer, breast cancer is the second leading cause of cancer deaths in women. According to the American Cancer Society, about 1.3 million women will be diagnosed with breast cancer. One woman under age 20 out of 1,985 will develop breast cancer; by age 30 the risk is 1 out of 229, by age 40 it is 1 out of 68, and so on, with a lifetime risk of 1 out of 8. Those statistics are frightening. Each of those numbers is a living, breathing human being, and there are few of us who have not been touched by the breast cancer diagnosis of a mother, grandmother, daughter, sister, cousin or friend.
There is evidence that the death rate from breast cancer has gone down in the past 25 years due to mammography, which results in early detection and treatment.
Many groups have sounded an alarm over the new guidelines, including the National Medical Association, the professional group which represents over 30,000 African American physicians, which was quick to respond.
The NMA released a statement Nov. 19 saying that African American women, in consultation with their physicians, should continue the previous practice of yearly mammograms starting at age 40. It said, “The NMA strongly recommends clinical breast exams, self-breast examinations, mammography and all other emerging technologies as important tools in prevention. The health care community has spent the last two decades promoting screenings and early detection. We do not want all of the progress that has been made in promoting screenings to be lost. The current screening guidelines while not perfect, do save lives.”
The NMA’s concern is derived from the fact that African American women tend to develop breast cancer at an earlier age than other demographic groups. Further, their cancers tend to be more aggressive, with a higher death rate.
While advocacy groups like the National Breast Cancer Coalition, Breast Cancer Action and the National Women’s Health Network endorsed the new guidelines, officials of the American Cancer Society and the American College of Radiology have said that they are recommending that women continue to follow the previous guidelines. Dr. Otis W. Brawley, chief medical officer of the American Cancer Society, said that the society’s medical experts had reviewed the data, that mammography has risks as well as benefits, but that the benefits of annual mammography outweigh the risks.
In making its recommendations, the task force weighed the benefits of mammography for women under age 50 against the risks. It found that one cancer death is prevented for every 1,904 women age 40 to 49 who are screened for 10 years, versus one death for every 1,339 women age 50 to 59, and one death for every 377 women age 60 to 69.
Since one in every eight American women will be diagnosed with breast cancer, the idea of not having every available technology available can be terrifying. When real, live human beings are involved, the one death in 1,904 takes on new meaning. Experts are advising women to consult their doctors when deciding how often to undergo mammography. It is recommended that some women, those with a strong family history of breast cancer, genetic markers for breast cancer, or a history of breast cancer, should without doubt receive yearly screenings, including mammography.
All this rings hollow if a woman does not have health insurance, or if there are no resources for free mammograms in her community. Also, it is not unheard of for a woman to receive a free mammogram, only to be unable to have further testing if the mammogram results indicate a problem.
Photo: commons.wikipedia.org www.cancer.gov












Comments